There is no particular time for PMS. It can start anytime from the time of ovulation until menstruation.
Almost 80-90% of women experience PMS in their lifetime. In most instances, mild to moderate l of disturbances will not affect daily life. However, the severe condition is called Premenstrual Dystrophic Disorder (PMDD). It is challenging to self-handle this condition and typically requires medical intervention.Â
The exact reason for PMS is yet unknown. However, reproductive hormonal changes and serotonin influences have found to be associated with it. A low level of serotonin (a hormone present in the brain and gut) affects the mood, emotions, and thoughts.
Risk factors for premenstrual syndrome
Anyone can get PMS, but certain risk factors can certainly trigger PMS. These include:
- Family history of PMS or depression
- Physical and/or mental trauma
- Abuse
- History of anxiety and depressive disorders
- Dysmenorrhea
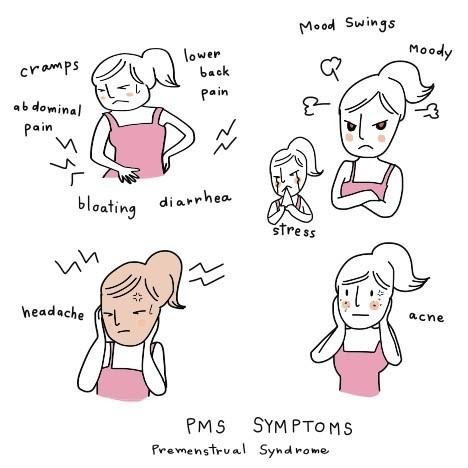
Symptoms of premenstrual syndrome
It is not like everyone will experience all the symptoms all the time. Two or three symptoms out of the following might be experienced in a month. Also, the symptoms for PMS are many, but the most common symptoms include:
Emotional symptoms
- Irritability
- Angry outbursts
- Anxiety
- Crying spells
- Depression
- Confusion
- Sleep problems like insomnia or frequent napping
- Poor concentration
- Social withdrawal
- Changes in sexual desire
Physical symptoms
- Breast tenderness
- Bloating
- Weight gain
- Food cravings
- Headaches
- Swelling of the hands and feet
- Aches and pains
- Fatigues
- Skin problems
- Abdominal pain
- Gastrointestinal symptoms
These symptoms can also be due to underlying depression and anxiety disorders. And sometimes, it can also start in premenopausal females.
Women can have superimposed premenstrual syndrome over depression and anxiety disorders.
The severity of PMS varies from person to person. Depending on your endurance level, you will have to decide to seek medical advice.Â
How to diagnose PMS?
. There is a pattern of symptoms that a woman notices:
- Symptoms occur during 5-7 days before the start of her menstrual cycles, and this happens for at least three cycles in a row. The symptoms end within four days.
- The symptoms hinder the day to day activities.
- A detailed record of menstruation dates, symptoms, how long they last, etc. will help the doctor to diagnose and provide a solution for the problem.
How to manage premenstrual syndrome?
There is no exact cure for PMS. However, it is possible to reduce the severity of the symptoms by adapting to a few changes in life. These include:
- Regular exercises – Being physically active will help to balance the hormone fluctuations. This helps to control mood swings, depression, anxiety, irritability, and sleep disturbances. It is found that regular 30-minute exercise sessions reduce PMS.
- Stress management and relaxation therapy help immensely in alleviating PMS. Relaxation therapy includes meditation, breathing exercises, and yoga. Massage therapy is another type of relaxation therapy that you may try.
- If self-relaxation does not help, one should take clinical psychologists’ help as sometimes hypnosis, and biofeedback therapy might help.
- Regular sleeping habit is an essential part of PMS prevention, which helps to lessen moodiness and fatigue.
- Hydrating well will prevent water retention and abdominal bloating.
- Taking vitamin supplements will help to reduce the symptoms by healing cramps and mood swings. Calcium and magnesium are found to be helpful too.
- Dietary Changes
- Eat a balanced diet to improve your overall health and improve the energy level.
- Reduce caffeine intake.
- Opt for small frequent meals.
- Avoid pure starch, too much salt, fat, and sugar.
- Add plenty of vegetables and fruits in your diet.
You may seek medical support if your symptoms are unbearable and affect your daily routine. Apart from lifestyle corrections, you may be advised with stress management classes or with antidepressant medications or hormonal medications depending on your condition’s severity.
Thus, a healthy lifestyle and a comprehensive treatment plan can reduce and control the symptoms of PMS and PMDD in most women.
Special thanks to Dr. Ragini Agrawal (MS, FICOG, FICMCH) for the expert advice.